Weizmann Institute researchers have developed a molecule that allows blood stem cells -- the body's most primitive and most immature cells, which originate in the bone marrow -- to multiply without maturation in the test tube.
This achievement may improve bone marrow transplantation, in which stem cells are infused into a patient to replace defective or malignant marrow. The study may also advance gene therapy research.
The new molecule was developed by Prof. Michel Revel and Dr. Judith Chebath of the Molecular Genetics Department, and its effects on blood stem cells were studied by Dr. Tsvee Lapidot and graduate students Orit Kollet and Ronit Aviram of the Immunology Department.
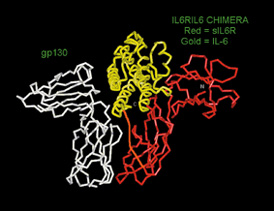
Most stem cells originating in the bone marrow mature daily to replenish our blood. A small number of stem cells, however, survive and renew themselves without maturation, thanks to a natural mechanism in which the cells receive signals from molecules called cytokines. Among these molecules is interleukin-6, a chemical messenger discovered in the 1980s in Revel's laboratory. In order to respond to interleukin-6, the stem cells form a cluster with this cytokine, consisting of a receptor molecule on their surface known as gp130 and another molecule called the interleukin-6 receptor, which the cells pick up from surrounding fluids.
In contrast, when isolated in the test tube, the stem cells do not efficiently form the cluster with interleukin-6 and fail to survive: They start to mature into various types of blood cells and lose their original properties within three to five days. This has caused the greatest difficulty in studying stem cells and using them for therapeutic purposes
In their study, Weizmann Institute scientists used a so-called "chimera" recombinant molecule, consisting of interleukin-6 and its receptor fused together. The "chimera" proved extremely efficient in spurring on the formation of clusters with gp130 on the surface of stem cells purified from human bone marrow or from human umbilical cord blood. When the chimera was added to isolated stem cells together with other cytokines, the cells were able to survive in the test tube for two weeks and their numbers increased significantly. In the future, this new approach may make it possible to keep the stem cells proliferating without maturation for much longer periods.
By transplanting the treated human stem cells into mice with severe combined immunodeficency, the scientists verified their ability to repopulate the bone marrow and produce all types of blood cells, demonstrating that the stem cells had indeed remained immature. A large increase in the efficacy of transplantation was observed with the stem cells that had received the chimera treatment compared with untreated cells.
If the Weizmann Institute molecule is adopted for clinical use, allowing stem cells to survive longer and increasing their numbers, the success of bone marrow transplantation can be improved. Such transplantation is currently used to treat an increasing number of diseases, including different types of leukemia and cancerous tumors, several blood cell disorders and even autoimmune diseases such as multiple sclerosis.
The Institute study may also provide a boost to gene therapy research by giving scientists a larger window of opportunity for inserting genes into human stem cells maintained in the laboratory. If scientists manage to do that, they may be able to develop gene therapy for various genetic disorders such as thalassemia, severe combined immuno?deficiency, Gaucher's disease, and other disorders. Since transplanted stem cells repopulate the bone marrow of the recipient and daily produce billions of blood cells, inserting a gene in these cells prior to transplantation would ensure a steady supply of the protein made by this gene, compensating for the genetic defect causing the disease.
The Institute scientists collaborated with researchers from the Bone Marrow Transplantation Center at the Hadassah University Hospital in Jerusalem, from the Kaplan Hospital in Rehovot and from the Jackson Laboratory, Bar Harbor, Maine.
 and Prof. Tsvee Lapidot (left).jpg)