Dr. Tsvee Lapidot is in a race to the finish. This is not a race to win a trophy, but to find a means of saving lives otherwise lost when bone marrow transplants just don't take.
"We discovered that human stem cells are something like sailboats," Lapidot of the Immunology Department says of his work. "A sailboat will pick up the wind only if its sail is hoisted to a mast. Similarly, stem cells will migrate to the bone marrow only if they display on their surface a specific receptor that allows them to pick up the signals from marrow cells."
In bone marrow transplantation, a patient receives a transfusion of stem cells; ideally these migrate to the patient's bone marrow and start producing new, healthy blood. But many transplants fail. Why? Usually, too few stem cells make their way from the blood circulation into the recipient's bone marrow.
Lapidot's research team has revealed key elements of the mechanism responsible for migration of stem cells from circulating blood to the bone marrow. Furthermore, the scientists managed to dramatically increase the proportion of stem cells capable of migrating to the marrow.
"In the future, this approach might improve the success rate of human bone marrow transplantation," Lapidot says. He conducted this research with Drs. Amnon Peled, Isabelle Petit, Orit Kollet, Ofer Lider and Ronen Alon, together with Prof. Dov Zipori of the Molecular Cell Biology Department.
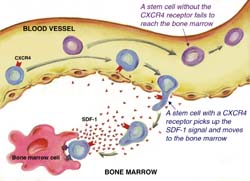
Bone marrow transplantation is a last-resort treatment that saves the lives of many patients with leukemia, other malignancies, and various blood disorders. In a transplantation, the patient's malignant or defective marrow is destroyed, and healthy stem cells are transfused intravenously into the blood circulation, in the hope that they will find their way to the patient's bones and create normal marrow. This marrow tissue daily produces hundreds of billions of red and white blood cells, the latter being those that protect the body from infections as part of the immune response. The Weizmann Institute scientists found that only human stem cells equipped with a certain type of receptor, called CXCR4, migrated from the circulation to the bone marrow of experimental mice. Aiding in this successful migration is a signaling molecule called SDF-1, which is released by bone marrow cells. To use another sailing metaphor, the signaling molecule is like a semaphore; it "attracts" human stem cells and guides them through the blood vessel walls into the marrow cavities.
The fact that only a small number of human stem cells display the CXCR4 receptor on their surface explains why so few stem cells are successfully transplanted. In the past, the low success rate was attributed to rapid stem cell differentiation. According to this theory, stem cells that entered the bone marrow cavity "disappeared" because, instead of proliferating, they quickly matured into the various types of blood cells. The new study, however, suggests that stem cells may also disappear because they lack the CXCR4 receptor and therefore fail to migrate to the recipient's marrow.
The researchers further demonstrated that the majority of human stem cells that do not express the CXCR4 receptor on their surface have the potential to do so. When, prior to transplantation, the stem cells were treated in a test tube with natural growth factors that stimulated them to express the CXCR4 receptor, they were converted into migrating cells capable of contributing to the daily production of blood. In the Weizmann study, use of this technique increased the number of successfully transplanted, functional human stem cells from 25 percent to more than 90 percent.
In the future, it may be possible to predict the success of a human bone marrow transplant by evaluating the highly variable proportion of the patient's stem cells that express the CXCR4 receptor. It may even be possible to preselect stem cells equipped with the CXCR4 receptor for transplantation purposes, or to pretreat the stem cells so that they all display the receptor.
These measures should significantly increase the overall success rate of the procedure. Clinical testing of the method is currently under consideration.
This study could be conducted thanks to an experimental system developed by Lapidot and his colleagues, which overcomes a major difficulty in studying human stem cells: In a test tube, they quickly differentiate into mature blood cells and disappear. Lapidot's team developed a way of studying human stem cells by transplanting them into immunodeficient mice that lack the ability to reject foreign cells. This animal model thus serves as a powerful tool for research that may lead to improved therapies for human leukemias and other disorders.
The study was conducted in collaboration with researchers and physicians from the Hadassah University Hospital in Jerusalem, the Kaplan Medical Center in Rehovot, the Sourasky Medical Center in Tel Aviv, and the Jackson Laboratory in Bar Harbor, Maine.
Yeda Research and Development Co. Ltd., the Weizmann Institute's technology transfer arm, has filed a patent application for the findings of Dr. Lapidot's team.