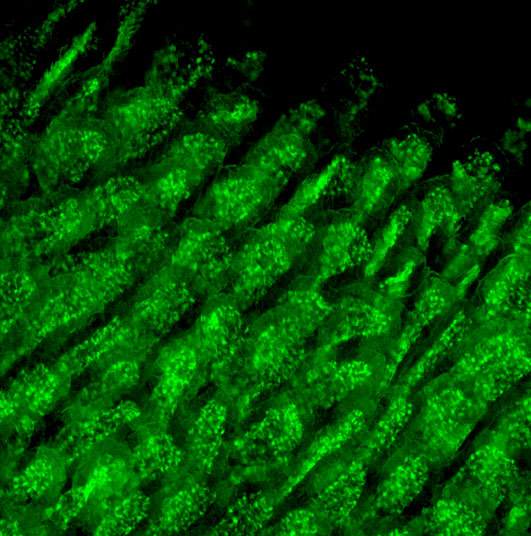
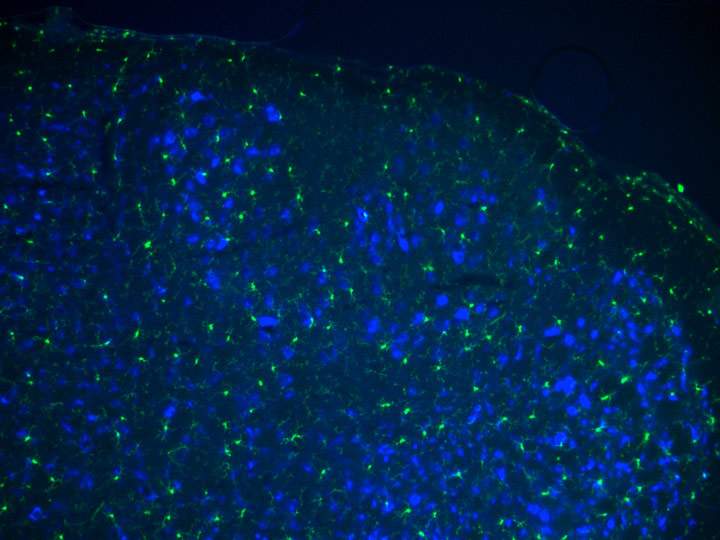
The tasks that the macrophages carry out in the various organs can be highly specific. In the nervous system, for example, they play a role in shaping nerve cells, while in the spleen they dine on well-aged red blood cells. Jung, who has been studying macrophages for a decade, recently revealed that, unlike most immune cells, many macrophages are long-lived cells that arise in the embryo, developing alongside their host organs. These findings raised new questions about macrophage development. For example, how do they get trained to serve each particular organ and tissue?
To begin to answer these questions, Jung joined up with departmental colleague
Dr. Ido Amit, who investigates how regulatory regions in the genome control immunity. There are only a handful of macrophages in any one organ, but Amit and his team have developed cutting-edge techniques, including advanced robotics and next-generation sequencing technologies, to study such rare, specialized cells in their natural state. The scientists profiled these cells down to the molecular level, using the data to explain the unique ways their genes are expressed and regulated.
The team, which also included Dr. Deborah Winter, Dr. Ronnie Blecher-Gonen, Eyal David and Dr. Hadas Keren-Shaul, all of the Weizmann Institute’s Immunology Department, and Yonit Lavin and Prof. Miriam Merad of the Icahn School of Medicine at Mount Sinai, New York, examined macrophages in seven different organs – from brain to lungs to intestines. They succeeded in identifying a unique signature for each of these populations, based on their genomic profiles and regulatory landscapes – a sort of textured map of their convoluted genetic activities. In particular, the team noted that each macrophage population used a distinct set of regulatory elements, or “enhancers,” for turning “on” or “off” the expression of certain genes.
Next the researchers switched these cells between organs. To their surprise, the macrophages began to change their signatures, taking on new profiles to fit their new surroundings. When the cells grew from immature cells, the revamping process was nearly complete – over 90%. But even when the experiment was repeated with fully differentiated cells, there were substantial changes in the macrophages’ personality profiles. Specifically, macrophages that were moved from the peritoneum to the lungs started to look and act like functional lung macrophages.
These findings, Amit and Jung believe, could change quite a few preconceived notions about macrophages. For one, these cells turn out to be incredibly plastic: “It’s a sort of ‘nature versus nurture’ issue,” says Winter, who led the study together with Blecher-Gonen. “Our findings suggest that nurture plays a much stronger role in shaping these cells’ identities than anyone had thought.” And the ways that the cells take their cues from their surroundings support Jung’s earlier findings: Macrophages arise from common precursor cells in the embryo and specialize after receiving signals from their host tissue, thus becoming an integral part of their surroundings. This goes beyond mere genetics, say the researchers: Understanding how the fate of such cells as macrophages is determined could help decipher the molecular mechanisms of diseases, including immunological disorders, anemia, leukemia and more.
The study was conducted in mice, but the ultimate goal is to apply the findings to humans. “In the future,” says Blecher-Gonen, “we want to learn how to retrain the macrophages ourselves. Then we could use them to treat diseases in which the patient’s macrophages are faulty or inadequate.” As an example, the team envisions creating lung macrophages that could clean up the thick secretions blocking the lungs of cystic fibrosis patients, or designer gut macrophages that could be used to treat irritable bowel disease. Amit: “Since most disease-causing mutations are located in regulatory regions, further studies could shed new light on the pathways involved in such diseases as inflammatory bowel disease and multiple sclerosis, and perhaps lead to the more precise treatment of patients.”
Ido Amit's research is supported by the M.D. Moross Institute for Cancer Research; the J&R Center for Scientific Research; the Jeanne and Joseph Nissim Foundation for Life Sciences Research; the Abramson Family Center for Young Scientists; the Wolfson Family Charitable Trust; the Abisch Frenkel Foundation for the Promotion of Life Sciences; the Leona M. and Harry B. Helmsley Charitable Trust; Sam Revusky, Canada; the Florence Blau, Morris Blau and Rose Peterson Fund; the estate of Ernst and Anni Deutsch; the estate of Irwin Mandel; and the estate of David Levinson. Dr. Amit is the incumbent of the Alan and Laraine Fischer Career Development Chair.
Prof. Steffen Jung's research is supported by the Leir Charitable Foundations; the Leona M. and Harry B. Helmsley Charitable Trust; the Maurice and Vivienne Wohl Biology Endowment; the Adelis Foundation; Lord David Alliance, CBE; the Wolfson Family Charitable Trust; the estate of Olga Klein Astrachan; and the European Research Council.