Recent Weizmann Institute studies are revealing a complex picture of cancer progression in which certain genes that drive tumor growth in the earlier stages get suppressed in later stages – taking a step back to move forward.
Current research in the lab of
Prof. Avri Ben-Ze’ev of the Molecular Cell Biology Department suggests that the tumor cells at the invasive front of later-stage human colorectal cancer may take an even bigger step back: Some of their gene expression patterns are shared with those of healthy intestinal stem cells.
Colorectal cancer is most deadly when the cancer has metastasized – spread to other organs in the body, mainly to the liver. Ben-Ze’ev and his team had previously discovered that a mutation found in 80% of all colorectal cancers leads to enhanced expression of another gene, called L1, especially in the cells at the leading edge of metastatic growth. L1 is known to play a role in cell-to-cell adhesion; in the present study, further investigation into L1 expression led the group to yet another gene, called SMOC-2.
The researchers investigated the role of this gene in mouse models of colorectal cancer metastasis to the liver, finding that L1 produced heightened SMOC-2 levels during this stage. When the researchers increased the levels of SMOC-2 in human colorectal cancer cells, their metastasis to the liver was fast and aggressive. Conversely, blocking the gene in colon cancer cells inhibited metastasis, conclusively indicating that the activation of SMOC-2 by L1 plays a crucial role in the spread of this cancer.
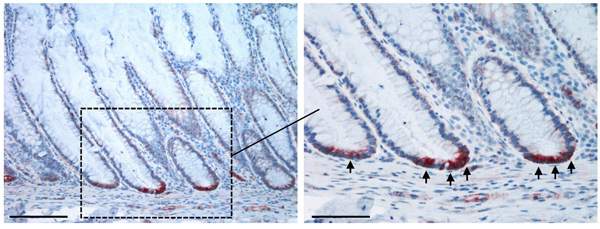
Similarly elevated SMOC-2 levels had been seen by another group – in mouse intestinal stem cells, which provide replacements for the cells in the intestinal walls. Ben-Ze’ev’s group found that SMOC-2 is normally expressed in the colon exclusively in the stem cells’ protected niches at the bottom of the tube-like “colon crypts.” In human colorectal cancer, in contrast, the gene was expressed in the more invasive regions of the tumor.
What does this gene do? SMOC-2 encodes a molecule that is secreted by the cells and then makes it way to the outer part of the cell membrane, where it facilitates movement. This molecule is thought to help differentiating stem cells disengage from their neighbors and make their ascent up the colon crypt walls. Similarly, metastatic human colon cancers seem to activate this gene to enable them to “leave home” and make their way out.
This research, says Ben-Ze’ev, provides support for the idea that as cancer develops it also reverts – that is, some of its cells adopt a less mature, more stem-like, state that assists metastasis. Additional investigations into the interactions between SMOC-2 and other genes suggested that the human cancer cells were, indeed, taking on some qualities of stem cells.
Ben-Ze’ev hopes that further research will point to ways of interfering with the activities of genes like SMOC-2, thus preventing this cancer from metastasizing. In addition, he says, the expression patterns of SMOC-2 could make it an ideal marker for the early detection of human metastatic colorectal cancer.
Prof. Avri Ben-Ze'ev is the incumbent of the Samuel Lunenfeld-Reuben Kunin Chair of Genetics.